
Un laboratoire sur fibre optique pour diagnostiquer les cancers in vivo
www.lemonde.fr
May 15, 2026, 2:18 p.m.
Analyser des cellules directement dans le corps d’un patient afin d’établir, de manière peu invasive, un diagnostic de cancer. Cet examen du futur réalisé à l’aide de capteurs multifonctions placés à l’extrémité d’une fibre optique est l’objectif de recherche d’une équipe multidisciplinaire.
Share on

Next-generation biosensing platforms: critical analysis of nanomaterial-enabled strategies and clinical translation
link.springer.com
May 10, 2026, 9:21 a.m.
Biosensor technologies are increasingly seen as important tools in healthcare diagnostics, especially for point-of-care (POC) and decentralized testing. A systematic comparison of sensing methods, the scattered integration of nanomaterials into unified designs, and the neglect of real-world usability factors like device miniaturization, user interface integration, and data sharing continue to be issues despite rapid advancements. This review critically examines recent progress in electrochemical, fluorescence, and colorimetric methods, with a special focus on signal amplification strategies using nanomaterials and their feasibility for real-world use.
Share on
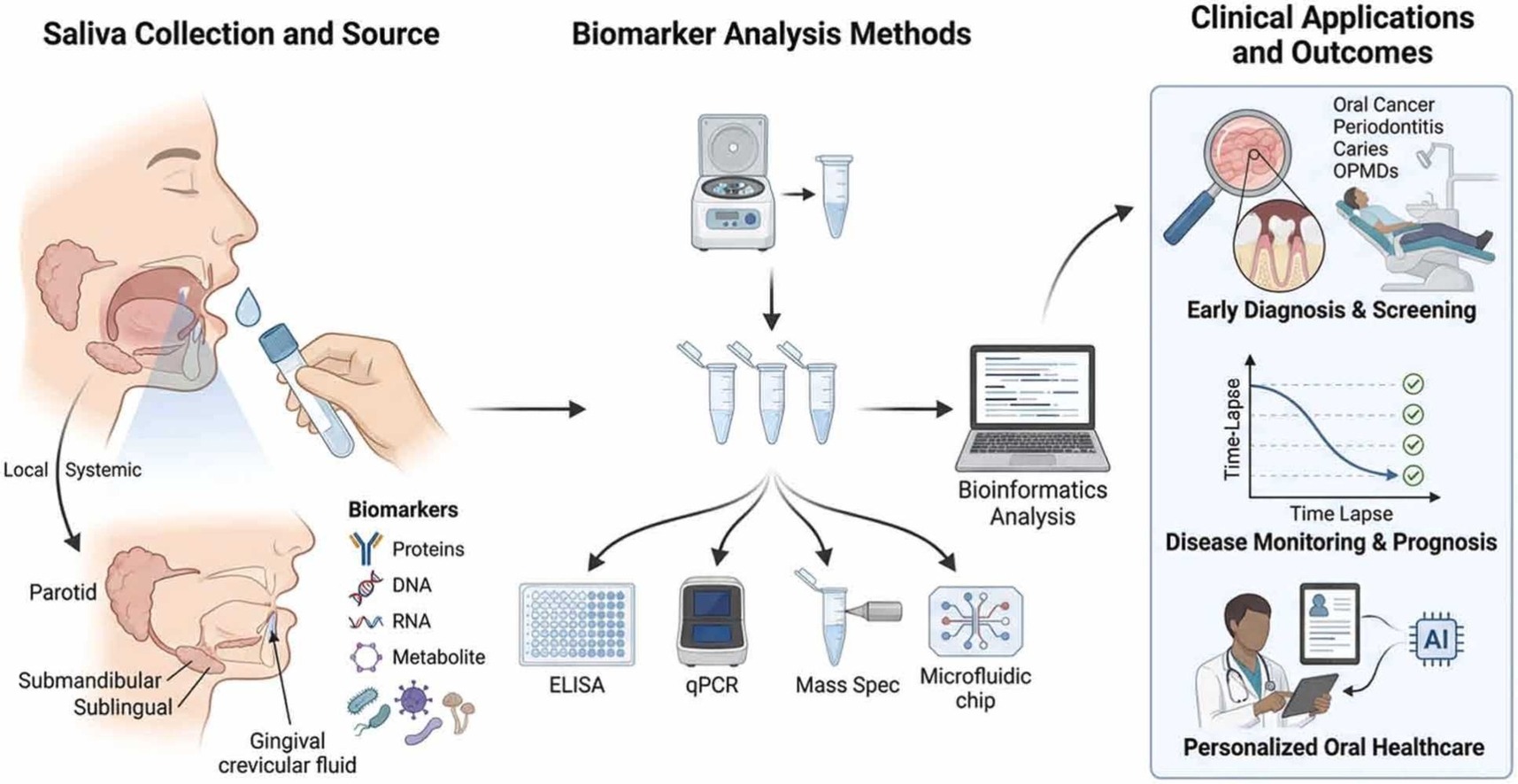
Salivary biomarkers and their diagnostic importance in oral diseases
www.sciencedirect.com
May 10, 2026, 9:17 a.m.
Salivary biomarkers enable non-invasive diagnosis and monitoring of oral diseases. Saliva omits and point-of-care tools improve sensitivity and clinical feasibility. Multi-omics and artificial intelligence drive future precision oral diagnostics.
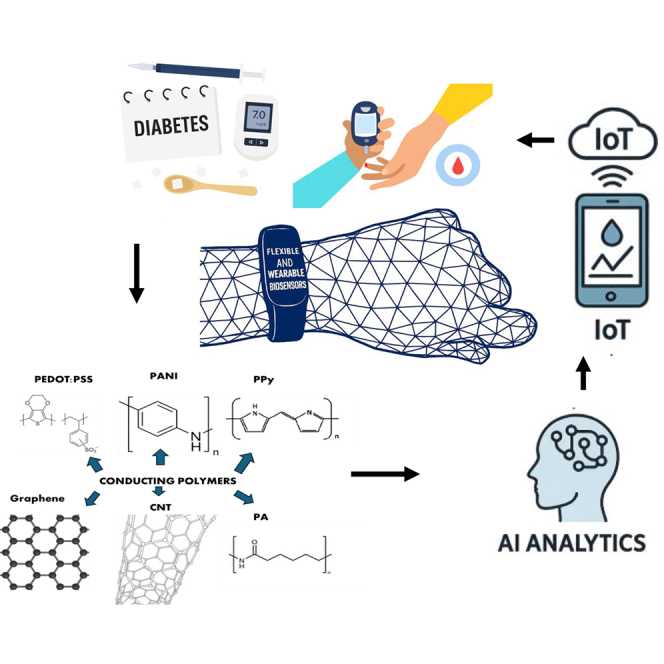
Flexible polymeric materials and wearable biosensors for smart ...
pmc.ncbi.nlm.nih.gov
May 9, 2026, 12:59 a.m.
This research explores the development and application of flexible polymeric materials and wearable biosensors for advanced diabetes mellitus diagnostics and continuous monitoring. The study addresses the critical need for non-invasive, real-time glucose monitoring solutions by leveraging innovative material science and sensor technology. Flexible polymeric substrates offer biocompatibility and mechanical adaptability, enabling seamless integration into wearable devices worn on the skin. These smart biosensors demonstrate potential for improving patient outcomes through enhanced diagnostic accuracy and personalized disease management. The investigation represents a significant advancement in point-of-care diagnostics and remote patient monitoring, with implications for transforming diabetes care delivery and enabling better disease surveillance in clinical and home settings.
Share on
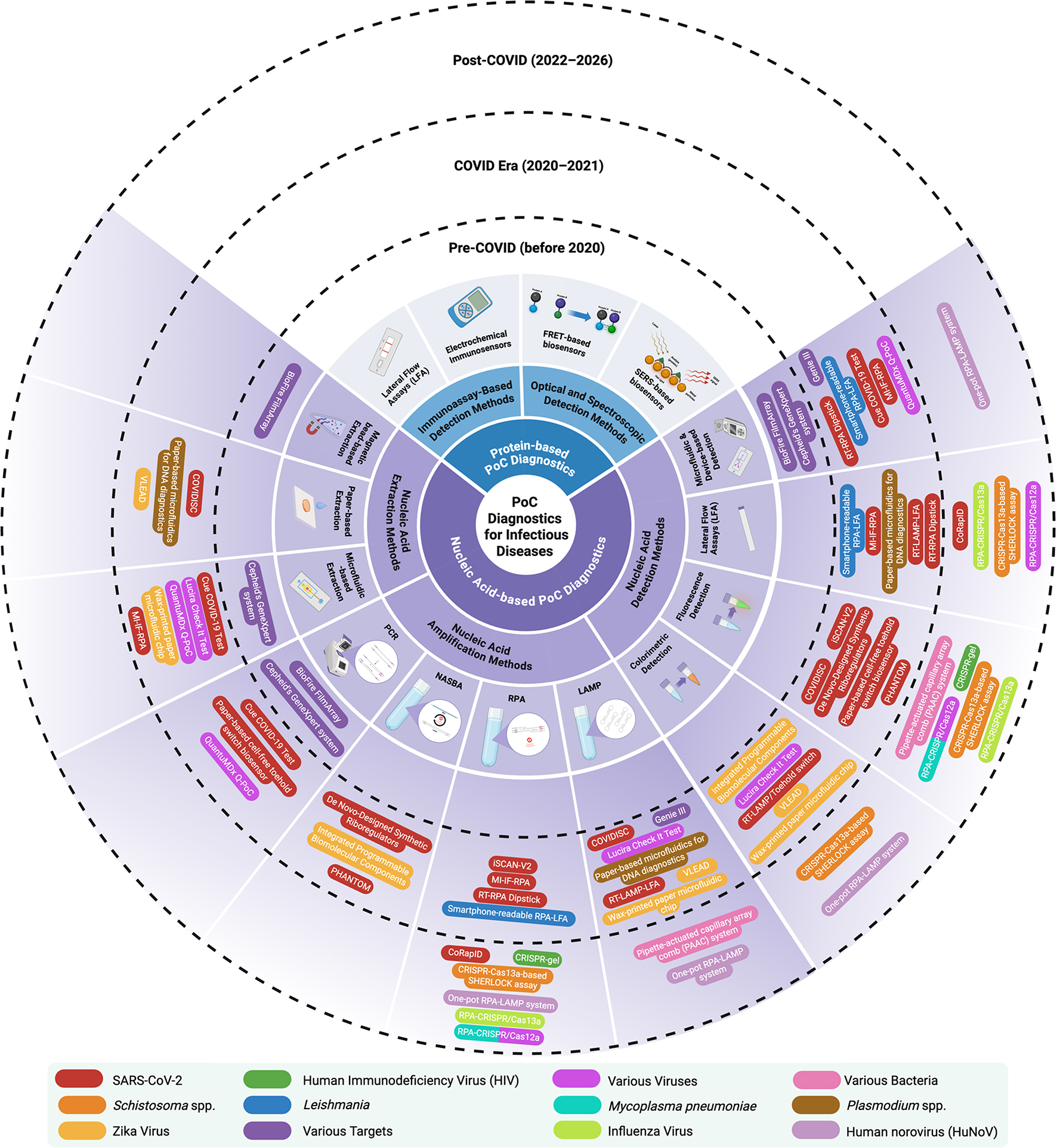
Trends of nucleic acid – based point-of-care diagnostics for ...
link.springer.com
May 9, 2026, 12:59 a.m.
This review examines nucleic acid-based point-of-care diagnostics for infectious disease detection, addressing the critical need for decentralized, accessible testing solutions. The article comprehensively explores three operational components: nucleic acid extraction, amplification, and detection across diverse platforms including lateral flow assays, biochips, and biosensors. It evaluates extraction strategies such as magnetic bead-based, paper-based, and integrated microfluidic approaches that prioritize simplicity and equipment-free operation. The review analyzes key amplification methodologies including PCR, NASBA, RPA, and LAMP, highlighting their modifications for rapid, low-power, and portable applications. These technologies collectively represent advancements in delivering sensitive, selective, and economically viable diagnostic testing outside traditional laboratory settings, enhancing global infectious disease surveillance and response capabilities.
Share on
Research Advances in the Application of Microfluidic Chip Technology for ...
www.frontiersin.org
May 9, 2026, 12:59 a.m.
Microfluidic chip technology represents a significant advancement in addressing the growing challenge of antimicrobial resistance by enabling rapid detection of antibiotic-resistant bacteria. Unlike conventional culture-based diagnostic methods that require several days and contribute to increased mortality and inappropriate antibiotic use, microfluidic platforms offer miniaturized, automated point-of-care solutions. Recent innovations have integrated bacterial isolation, phenotypic susceptibility testing, and genotypic resistance detection into self-contained lab-on-a-chip systems that minimize contamination and operator dependency. These sophisticated platforms operate at single-cell resolution, enabling detection of heteroresistance and resistant subpopulations that conventional bulk assays typically overlook, thereby providing clinically actionable results more rapidly and supporting more effective antimicrobial stewardship.
Share on

Microfluidic advances in biosensing, biofabrication, and next generation ...
www.nature.com
May 9, 2026, 12:58 a.m.
Microfluidic technology is revolutionizing biosensing, biofabrication, and microscale chemical processing. Wearable microfluidic platforms enable continuous, non-invasive health monitoring through real-time biofluid analysis, significantly enhancing point-of-care diagnostics accuracy and scope. In biofabrication, three-dimensional bioprinting and droplet-based microfluidics provide sophisticated tools for creating tissue engineering systems, drug delivery platforms, and advanced biomaterials with precisely controlled properties. High-performance microreactors simultaneously facilitate high-throughput screening and controlled biochemical reactions in compartmentalized environments, advancing reaction engineering and process modeling. This comprehensive collection showcases integrated innovations spanning wearable diagnostics, droplet methodologies, and compartmentalized biochemical approaches, demonstrating microfluidics' transformative potential in healthcare and biomedical applications aligned with sustainable development goals.
Share on

HMB is more common than asthma or diabetes, yet often ignored
news.harvard.edu
Oct. 8, 2025, 3:45 p.m.
Women with heavy menstrual bleeding wait five years on average for care. Wyss technology could change that.
Share on
New microfluidic device brings affordable kidney testing to the point of care
www.news-medical.net
June 3, 2025, 8:23 a.m.
Chronic kidney disease (CKD) affects over 800 million people globally and is often diagnosed too late for effective intervention. Early detection depends on accurate measurement of biomarkers such as creatinine and the urine albumin-to-creatinine ratio (uACR). While urine testing is non-invasive and informative, standard methods are time-consuming, costly, and require specialized facilities. Existing point-of-care devices offer convenience but remain prohibitively expensive or technically complex for many users. As such, there is an urgent need for a robust, affordable, and easy-to-use platform to measure urinary creatinine with clinical precision.
Share on
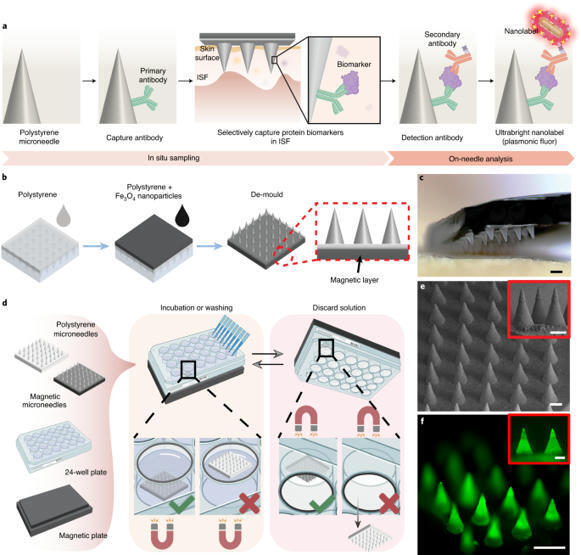
Microneedle patch for the ultrasensitive quantification of protein biomarkers in interstitial fluid
www.nature.com
March 12, 2025, 5:51 p.m.
The detection and quantification of protein biomarkers in interstitial fluid is hampered by challenges in its sampling and analysis. Here we report the use of a microneedle patch for fast in vivo sampling and on-needle quantification of target protein biomarkers in interstitial fluid. We used plasmonic fluor—an ultrabright fluorescent label—to improve the limit of detection of various interstitial fluid protein biomarkers by nearly 800-fold compared with conventional fluorophores, and a magnetic backing layer to implement conventional immunoassay procedures on the patch and thus improve measurement consistency.
Share on

DNA testmaker BillionToOne claims billion-dollar valuation with $130M funding round
www.fiercebiotech.com
March 4, 2025, 3:12 p.m.
BillionToOne said that since launching its first tests in 2020, over 500,000 patients have been evaluated to date, driving $125 million in annual revenue.
Share on

FDA, Gates Foundation team up on breath-based diagnostic tests
www.fiercebiotech.com
March 4, 2025, 3:08 p.m.
The FDA has launched a project with the Bill and Melinda Gates Foundation to help aid the development of breath-based diagnostics for detecting diseases more easily among underserved populations. The TB-focused project with the FDA follows up on the Gates Foundation's interest in breath biopsy tests developed by Owlstone Medical.
Share on

Flavored lollipops may offer non-invasive mouth cancer detection
interestingengineering.com
March 25, 2024, 11:59 a.m.
Diagnosing mouth cancer often involves invasive and uncomfortable procedures like biopsies and nasoendoscopy (inserting a flexible tube with a camera into the nose or mouth). However, scientists at the University of Birmingham are paving the way for a more patient-friendly approach – flavored lollipops that could potentially detect mouth cancer. This innovative research has garnered significant support, with Cancer Research UK and the Engineering and Physical Sciences Research Council providing £350,000 in funding.
Share on
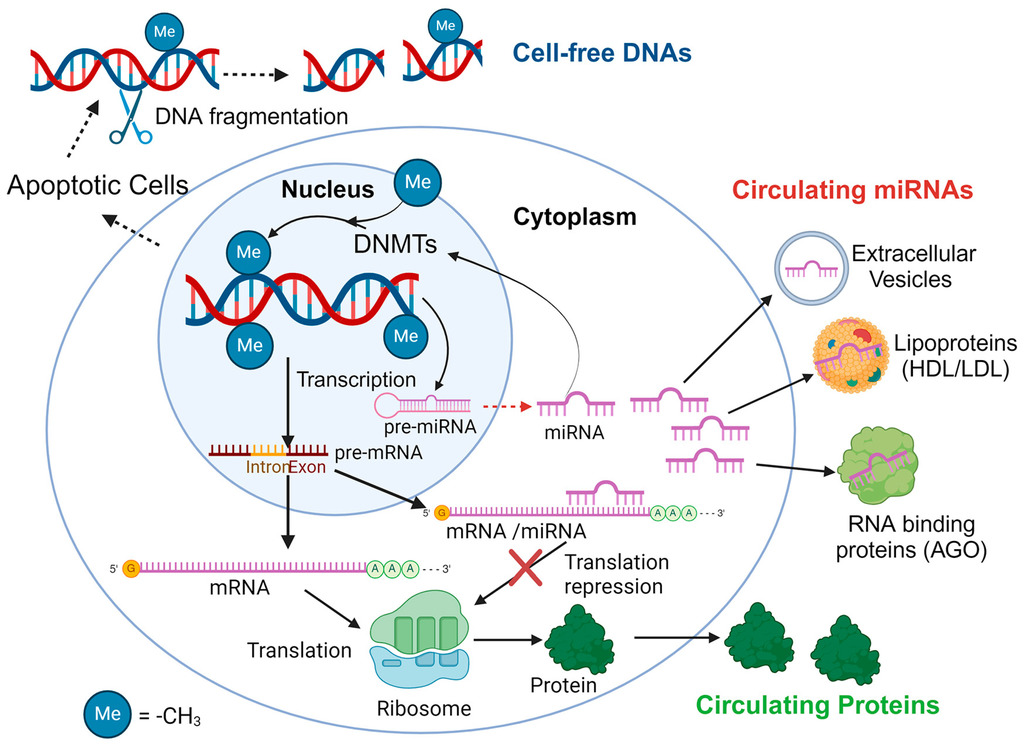
The Circulating Biomarkers League: Combining miRNAs with Cell-Free DNAs and Proteins
www.mdpi.com
March 18, 2024, 8:18 a.m.
The potential of liquid biopsy for the prognosis and diagnosis of diseases is unquestionable. Within the evolving landscape of disease diagnostics and personalized medicine, circulating microRNAs (c-miRNAs) stand out among the biomarkers found in blood circulation and other biological fluids due to their stability, specificity, and non-invasive detection in biofluids. However, the complexity of human diseases and the limitations inherent in single-marker diagnostics highlight the need for a more integrative approach. It has been recently suggested that a multi-analyte approach offers advantages over the single-analyte approach in the prognosis and diagnosis of diseases. In this review, we explore the potential of combining three well-studied classes of biomarkers found in blood circulation and other biofluids—miRNAs, DNAs, and proteins—to enhance the accuracy and efficacy of disease detection and monitoring. Initially, we provide an overview of each biomarker class and discuss their main advantages and disadvantages highlighting the superiority of c-miRNAs over the other classes of biomarkers.
Share on

23andMe’s Fall From $6 Billion to Nearly $0
www.wsj.com
Feb. 3, 2024, 5:57 p.m.
Five years ago, 23andMe was one of the hottest startups in the world. Millions of people were spitting into its test tubes to learn about their ancestry. Oprah had named its kit one of her favorite things; Lizzo dressed up as one for Halloween; Eddie Murphy name-checked the company on “Saturday Night Live.” 23andMe went public in 2021 and its valuation briefly topped $6 billion. Forbes anointed Anne Wojcicki, 23andMe’s chief executive and a Silicon Valley celebrity, as the “newest self-made billionaire.” Now Wojcicki’s self-made billions have vanished. 23andMe’s valuation has crashed 98% from its peak and Nasdaq has threatened to delist its sub-$1 stock. Wojcicki reduced staff by a quarter last year through three rounds of layoffs and a subsidiary sale. The company has never made a profit and is burning cash so quickly it could run out by 2025.
Share on

New Eye Clock Predicts Aging Through Fluid Proteins
neurosciencenews.com
Oct. 25, 2023, 12:47 a.m.
Researchers have pioneered a method to measure ocular aging by studying proteins in eye fluid. Using artificial intelligence, they crafted an “eye-aging clock” from 26 out of nearly 6,000 proteins which can forecast aging. Their findings can lead to more personalized medical treatments and help in understanding disease triggers. The team aims to employ this method to other body fluids, enhancing drug development for various ailments.
Share on
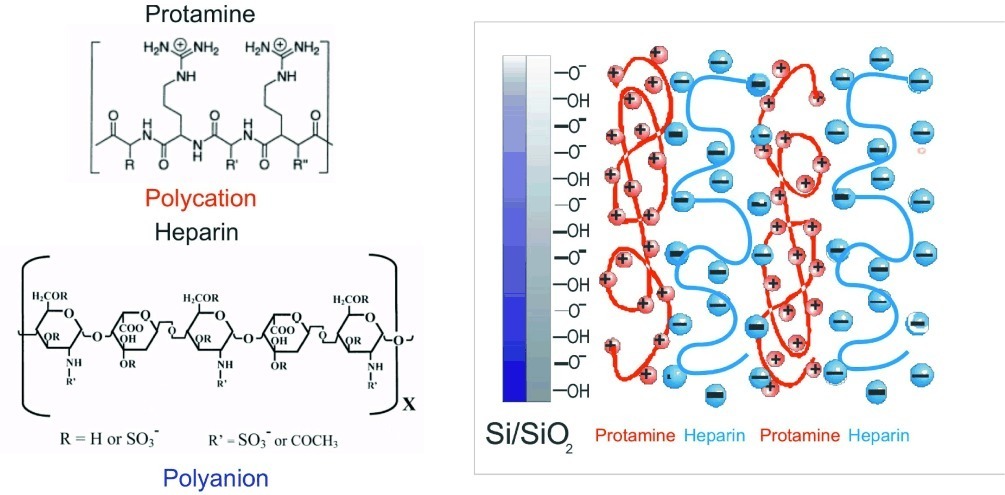
Title Monitoring Protamine‐Heparin Interactions Using Microcapillary Impedimetric Sensor
analyticalsciencejournals.onlinelibrary.wiley.com
Aug. 20, 2023, 12:03 p.m.
We report an impedimetric sensor based on an interdigitated electrode array with electrode digits located at the bottom of microcapillaries formed in silicon dioxide which is used to monitor protamine-heparin interactions. Modification of the active sensor surface with protamine, a cationic protein used as a high affinity heparin antagonist, permits to register protamine-heparin complex formation as changes in the surface conductivity determined from the sensor impedance measured in an electrolyte solution.
Share on

The DermaSensor device promises to aid providers in the detection of skin cancer
faimglobal.org
Aug. 12, 2023, 3:34 p.m.
Skin cancer is a prevalent cancer in the US. Detecting it is a pressing need. The FDA granted breakthrough device designation to The DermaSensor, a device that helps identify suspicious lesions for skin cancer. The DermaSensor is a non-invasive device that works by spectrometry. This device captures the substructure image of the cells and, together with software powered by machine learning, yields in just seconds an analysis of the nature and characteristics of the lesion.
Share on

Ultraflexible tattoo electrodes for epidermal and in vivo electrophysiological recording
www.cell.com
March 21, 2023, 5:55 a.m.
Tattoo electronics, flexible patches that mount directly onto the skin with the ease and flexibility of a temporary tattoo, have foreseen remarkable application potentials in personalized healthcare monitoring and human-machine interfaces. Documented tattoo electronics mostly have an on-skin form factor to date. Using dermal tattoos for in vivo diagnostics presents an unexplored paradigm. Here, we extend the application scenario of “tattoo electrodes” from an on-skin fashion to an actual under-skin configuration, enabled by a highly soft, conductive, and biocompatible polymer matrix.
Share on

Wrist-worn device can accurately predict troponin-I and obstructed arteries in five minutes
www.news-medical.net
March 13, 2023, 1:57 a.m.
The results indicate that the system predicts troponin-I levels with about 90% accuracy. In addition, the findings correlated well with clinical evidence of a heart attack; people with abnormal troponin levels as measured by the device were about four times as likely to have an obstructed artery compared to people with a negative troponin result as measured by the device. Download source article at: https://www.researchgate.net/publication/369076645_A_Novel_Breakthrough_in_Wrist-Worn_Transdermal_Troponin-I-Sensor_Assessment_for_Acute_Myocardial_Infarction/fulltext/64088c2f0d98a97717ec869f/A-Novel-Breakthrough-in-Wrist-Worn-Transdermal-Troponin-I-Sensor-Assessment-for-Acute-Myocardial-Infarction.pdf
Share on